 |
| State Dept. for Public Health graph, adapted by Kentucky Health News; to enlarge, click on it. |
Kentucky Health News
As Kentucky came close to leaving the statewide "red zone" for coronavirus infection, Gov. Andy Beshear told state employees they could take off their masks and made the state's guidance for school districts – which seem to have largely dropped mask mandates – conform to new federal guidelines.
From Saturday to Monday, the state reported 2,754 new cases of the coronavirus, reducing the seven-day rolling average to 1,889, about half what it was just 10 days ago.
In the Monday-to-Sunday reporting week ended Feb. 27, Kentucky reported 13,305 virus cases, just over half the 25,173 reported the previous week.
In the same reporting week, the average positive-test rate fell to 9.01%. The rate Monday was 8.56%. Beshear said Kentucky is seeing a steady positivity rate decline of about one-half point per day.
"The metrics are all continuing to move in the right direction, and they're moving very quickly in the right direction," Health Commissioner Steven Stack said at Beshear's weekly pandemic press briefing.Beshear said, "The pace of the decline continues to be significant. We want to continue to see these numbers going down. Right now, there's no reason to think that they won't."
The governor said that with a few exceptions in congregate settings, state government is moving to a mask-optional policy, which will also apply to visitors.
Beshear and Stack reviewed the Centers for Disease Control and Prevention's new masking guidance that is based on three indicators: cases in the past seven days, Covid-19 hospital admissions, and share of staffed beds occupied by Covid-19 patients. Those numbers rate each county as low, medium or high risk, with recommendations to fit.
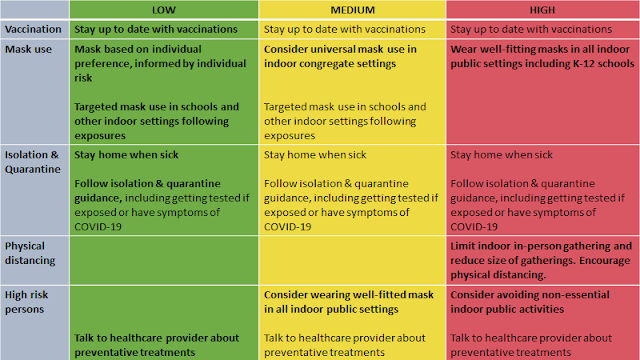 |
| New Centers for Disease Control and Prevention guidelines for Covid-19 prevention; click to enlarge |
In the 18 counties at medium risk, it says people who are immunocompromised or at high risk for severe illness should talk to a health-care provider about "additional precautions, such as wearing masks or respirators indoors in public. If you live with or have social contact with someone at high risk for severe illness, consider testing yourself for infection before you get together and wearing a mask when indoors with them."
Asked about likely compliance with this new guidance, Beshear said, "We always say that having more specific and more targeted guidance will help with compliance. We just need a commitment by our local leaders, but also all our individual families."
Starting next week, Stack said the state will switch to a weekly Covid-19 update that will coincide with the CDC's weekly update of the risk map: "It's much more appropriate as we look to start the third year of the pandemic. It gives timely information but it's also responsive to the realities of where we are."
Stack said his Department for Public Health is updating its school guidance to align with new CDC guidance that will make masks optional in schools in areas with low virus transmission, with targeted mask use following at-school exposures. The guidance will also recommend that schools in areas with medium transmission should consider universal masking for all students and staff and those in high transmission areas should require universal masking.
The CDC no longer requires masks to be worn on school buses. Stack said over the next couple of weeks, Kentucky schools will adjust their bus guidance to match what they are doing in classrooms.
Stack encouraged parents to get their school-aged children vaccinated, in part to prevent Multisystem Inflammatory Syndrome. He said about 100 Kentucky children have been diagnosed with this rare but serious condition that can occur two to six weeks after a Covid-19 infection, even in children who have mild infections or no symptoms at all.
Stack said he shared this information because more and more evidence is showing that vaccines largely prevent MSIS: "So please, our vaccination rates remain lowest in the school aged children. I would urge parents to be thoughtful about that, talk with your pediatrician and get your children vaccinated."
Twenty-one percent of today's new Covid-19 cases were in children.
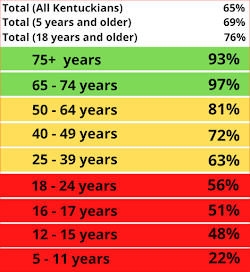 |
| Kentucky Department for Public Health table |
CDC data reported by The Washington Post says that in the last week, Covid-19 vaccinations in Kentucky averaged of 2,918 per day. That which up a bit from Saturday, when the average was 2,508, but still a 46% decrease from the week before.
"If there's one negative piece of information today," Beshear said, "it's that our vaccination numbers are dropping about as quickly as the virus itself."
The state's seven-day infection rate is 27.79 daily cases per 100,000 residents, barely in the "red zone" for a high level of transmission, above 25 per 100,000. But many counties still have very high rates.
Counties with rates more than double the statewide rate are Wolfe, 161.7; Perry, 153.1; Menifee, 118.9; Leslie, 105.6; Robertson, 88.1; Lawrence, 84.9; Knott, 80.1; Letcher, 76.9; Wayne, 76.6; Owsley, 74.4; Crittenden, 73; Martin, 72.7; Breathitt, 71.3; Morgan, 69.8; Bath, 69.7; Magoffin, 69.3; McCreary, 68.8; Jackson, 66.5; Lee, 65.6; Floyd, 63; Clay, 56.7; Anderson, 55.9; and Montgomery, 55.8.
Kentucky's infection rate continues to rank sixth among states, even with a 53% decline in cases in the last 14 days, according to The New York Times.
The state's Covid-19 hospitalization rate is second only to West Virginia's, but Kentucky's hospitals continued to get relief from the pandemic. They reported 962 patients with Covid-19 Monday, just over half the number reported two weeks ago, with 203 in intensive care and 112 on mechanical ventilation.
Six of the 10 hospital regions are using at least 80% of their intensive-care beds, with three over 90%. Beshear said 388 National Guard members are still helping hospitals and food banks, but probably won't be needed after March 15.
Asked about the legislation by Sen. Donald Douglas, R-Nicholasville, to end the Covid-19 state of emergency on March 7, Beshear said "We still have a pandemic" that can't be ignored and we don't need to "do anything that could stop us at any point from getting reimbursement for things that we need."
He said the bill "is more about politics . . . as far as I can tell from the outside . . . individual elections and pressure that people are facing." Douglas, who won a special election in November, is running in the May 17 primary election against Andrew Cooperrider of Lexington, who flouted Beshear's emergency pandemic restrictions and led protests against them.
From Saturday to Monday, Kentucky attributed 98 more deaths to Covid-19, bringing its pandemic death toll to 13,856. Beshear said two of the dead were in their early 20s and five were in between 39 and 49.
"Remember," he said, "we're still losing people that are far too young."




















