|
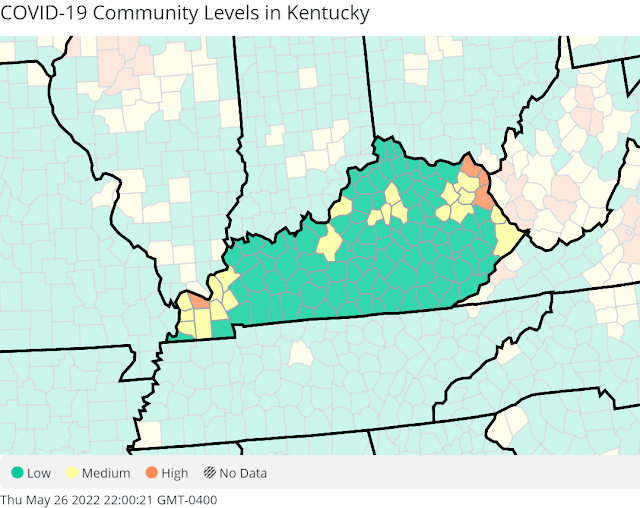
| Photo from The Lane Report |
Just like the rest of the nation, Kentucky needs more doctors, and people and institutions in the state are working on several initiatives to address the challenge.
The report cites several reasons: demand for services increases as the population ages and grows larger; many physicians are nearing retirement age; and the demands of the pandemic will accelerate retirements.
The pandemic has also raised awareness of the disparities in health care, emphasizing the need for more access to care, meaning we need more doctors.
For
The Lane Report, a Lexington-based business magazine, Jeff McDanald
reported how Kentucky's medical schools are stepping up to meet the challenge.
Kentucky ranks 40th among the states in primary-care physicians per 100,000 people, with only 2,696 practicing statewide, McDanald reports.
“There is certainly a maldistribution of primary care providers, with four of our counties (Ballard, Metcalfe, Owsley and Robertson) having no primary care physician and eight others (Bath, Carlisle, Edmonson, Hancock, Hickman, Nicholas, Spencer and Webster) having only one,” Dr. John Lee Roberts, vice dean for graduate and continuing medical education at the University of Louisville School of Medicine, told McDanald. “And 75 of our 120 counties are classified as primary-care health-profession shortage areas.”
One way U of L has worked to improve these numbers is offering scholarships to help offset medical-school debt.
“The average student-loan indebtedness of a graduating medical student is now well over $200,000,” Roberts told McDanald. “A partnership with the
Greater Louisville Medical Society has been generating five or six scholarships per year for University of Louisville students.”
U of L and the
University of Kentucky have also secured more Medicaid support for graduate medical education in the state, which has led to more resident and fellow positions in the past few years, which is key to alleviating the doctor shortages, McDanald reports.
However, Dr. Mark Newman, executive vice president of health affairs at UK, told Kentucky Health News that while the Centers for Medicare and Medicaid Services has increased funding for residency slots, it is not enough.
"UK welcomes this important funding; however, we estimate that it will likely result in just five additional slots for UK over five years," Newman said in an e-mail. "We will continue to work with our national associations on the need for additional funding for graduate medical education."
McDanald reports that the state’s three medical schools combined graduate about 500 students each year, but there are only about 400 entry-level residency positions in the state.
“Kentucky is a net exporter of doctors,” Roberts said. “We need more entry-level residency positions in Kentucky, and that starts with funding. . . . This is important because we have good data that shows 45 percent of the students who go to medical school in-state will ultimately practice in the state. Similarly, 45% of the residents and fellows who do their residency and fellowship in the state will ultimately practice in the state. But if you have Kentucky medical students who stay in Kentucky for residency and fellowship training, the numbers increase significantly to 74% of them who will end up practicing in the state.”
Role of economic development
Dr. Brent Wright of Glasgow, who has spent his career at a rural family medicine training program, told McDanald that while it is medical schools' responsibility to train residents, it is the responsibility of hospitals and communities to recruit them. Wright is associate dean for rural health and as an associate professor of family and geriatric medicine at U of L.
“Some communities do an extremely good job of referring physicians and are well aligned to their local government, but I think some places struggle,” Wright told McDanald. “When you recruit a physician you recruit the spouse, who may also want to work in the community. And if they have children, they’re looking for a good school system.”
“The ultimate placement of a physician in a community is really a team sport,” Wright said. “Communities need good infrastructure. This gets back to economic development, and if you have areas that start to become depressed, it’s really hard to reverse that.”
Geographic challenges
Dr. Charles H. Griffith, acting dean of the UK medical school, talked to McDanald about the need for physicians in rural parts of the state, especially when it comes to mental-health care.
"Kentucky is one of the worst states for under-served areas," Griffith told McDanald. "In some areas like Lexington and Louisville we probably do have sufficient doctors, but in our rural areas—which is a lot of the state—there is a dire need. We need primary-care doctors everywhere, but to be honest, there is a need for some of the general specialists out in rural areas.”
Griffith added that there is a great need for more psychiatrists in Kentucky.
“It’s especially evident with the mental-health crisis that’s been exacerbated by the pandemic,” he said. “There are just not enough psychiatrists to meet the mental health needs of children and adults, too.”
Griffith also noted that other health care providers, like nurse practitioners and physician assistants, are meeting some of the need to provide health care in Kentucky, noting that they "can do quite a bit."
Home-grown rural doctors
Another approach to get more physicians to practice in rural areas is to recruit rural medical students and provide rural residency programs, which is what the UK's Rural Physician Leadership Program aims to do.
“The program is based on the idea that it’s sometimes difficult to transplant someone into an underserved or rural area who is not familiar with the community,” Dr. Rebecca M. Todd, who heads the program in Morehead, told McDanald. “So instead, we go with the opposite approach of recruiting young men and women right out of these communities to go to medical school. Therefore, they are in tune with that patient population, they love the community, and they want to live and work there. It’s been a phenomenally successful program."
So much so that UK has now opened two larger regional campuses in Bowling Green and Northern Kentucky, McDanald reports.
The University of Pikeville's Kentucky School of Osteopathic Medicine has also helped to supply primary-care physicians to rural areas.
“Pike County used to be a medically underserved area and is no longer such because of the number of physicians who have come back to the area or have been attracted to the area partly due to the medical school being here,” Dr. Joe Kingery, dean of the osteopathic school, told McDanald.
Kingery told McDanald that 83% of UPike osteopathic graduates practice in primary care and stay in Kentucky, which exceeds the percentages for UK and U of L medical-school graduates.
“We have 57% of our graduates who are practicing in a rural area in Kentucky,” Kingery said. “It speaks to our story that we’re placing primary care physicians into underserved areas and the Appalachian region.” Kingery said. “That being said, our graduates can go into any specialty they want. We have orthopedic surgeons, neurologists, neurosurgeons, you name it. In a given year, we usually graduate about 125 to 130, with 65% to 70% of our graduates going into a primary care residency program. And for us, primary care is defined by only three specialties: family medicine, internal medicine and pediatrics.
In January, Campbellsville University welcomed the first class of students to its School of Chiropractic, the first in Kentucky and the only one within a 300-mile radius. It's in Harrodsburg.
“We’re responding to the doctor shortage by graduating doctors of chiropractic trained much like any physician as a port-of-entry care provider," Dr. Trevor Foshang, dean of chiropractic education, told McDanald.



,%20baby%20formula.jpg)